Comparison of immediate and mid-term outcomes of Blalock-Taussig shunt versus right ventricular outflow tract stenting in symptomatic neonates with tetralogy of Fallot
pp. 23-28
DOI:
https://doi.org/10.7775/rac.es.v90.i1.20474Keywords:
Tetralogy of Fallot - Stent - Blalock-Taussig Procedure - Anastomosis, Surgical - Heart Defects, CongenitalAbstract
Background: The initial management of neonate patients with tetralogy of Fallot (TOF) associated with an unfavorable anatomy
and significantly reduced pulmonary vascular flow is controversial and continues to be a clinical challenge.
Objective: The aim of this study was to describe the clinical evolution and to compare pulmonary artery branch development
in symptomatic neonatal TOF patients who received a modified Blalock Taussig shunt (mBT) versus right ventricular outflow
tract stent placement (RVOTs) at the Department of Cardiology, Hospital de Niños de Córdoba, between March 2011
and March 2021.
Methods: A retrospective, observational study identified 113 patients with TOF, 20 of which (18%) were symptomatic neonates
requqiring initial palliative intervention. Categorical variables are expressed as percentage and continuous variables
as median and interquartile range (IQR). A p value <0.05 was considered significant.
Results: Among the 20 patients included in the study, 11 (55%) formed the mBT group and 9 (45%) the RVOTs group. In
the mBT group, pre-palliative procedure right pulmonary artery (RPA) Z score was -3 (IQR 4.20) and increased to -1.6 (IQR
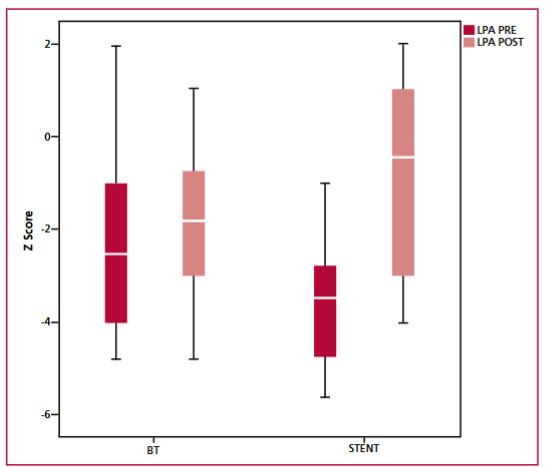
1.56) (p = 0.11) and left pulmonary artery (LPA) Z score of -2.5 (IQR 4.8) increased to -1.80 (IQR 2.36) (p = 0.44). In the
RVOTs group, RPA Z score prior to palliative intervention was -3.45 (IQR 3.83) and increased to -2.5 (IQR 3.58) (p = 0.021)
and LPA Z score of -4.10 (IQR 2.51) to -2.00 (IQR 3.75) (p = 0.011). Pre-intervention peripheral O2 saturation of 75% (IQR
6) increased to 87% (IQR 9) in the mBT group (p= 0.005) and from initially 75% (IQR 16) to 91% (IQR 13) in the RVOTs
group (p= 0.008). Mean hospital stay after the procedure was 10 days (IQR 11) in the mBT group and 6 days (IQR 2) in the
RVOTs group (p= 0.095).
Conclusions: In symptomatic neonates with TOF, both palliative strategies improved the clinical condition. In patients who
received RVOTs, there was greater development of pulmonary artery branches. A larger number of cases and longer-term
follow-up will be necessary to confirm these findings.
How to cite this article:
Rocchia F, Allub A, Guevara AA, De Anquín L, Juaneda I, Contreras A, et al. Immediate and Mid-term Outcomes of Blalock-Taussig Shunt versus Right Ventricular Outflow Tract Stenting in Symptomatic Neonates with Tetralogy of Fallot. Rev Argent Cardiol 2022;90:23-8. http://dx.doi.org/10.7775/rac.v90.i1.20474